The design and layout of the operating room directly affect surgical efficiency, patient safety, staff workflow, and infection prevention.
A well-designed operating room provides a sterile, functional, and ergonomic environment that supports complex surgical procedures while minimizing contamination risks.
As medical technologies and surgical techniques continue to evolve, hospitals must carefully consider multiple factors when planning or upgrading operating room facilities.
1. Importance of Proper Operating Room Design
A well-designed operating room supports safe and efficient surgical procedures. Poor design can lead to workflow interruptions, contamination risks, and reduced productivity.
The main goals of operating room design include:
- Maintaining a sterile environment
- Supporting efficient workflow for surgical teams
- Providing adequate space for advanced medical equipment
- Ensuring patient and staff safety
- Allowing easy cleaning and infection control
Hospitals today are increasingly adopting modular operating room systems, which use prefabricated components installed in controlled factory environments and assembled on-site. These systems help standardize layout, improve hygiene, and simplify future upgrades.
2. Operating Room Size and Space Requirements
Operating rooms must provide sufficient space for surgical teams, equipment, and patient movement. Operating room size is determined by the specific surgical procedures performed within it.
Typical operating room sizes include:
- Standard operating room: 400–600 sq ft (37–56 m²)
- Specialized OR (cardiac, neurosurgery): 600–800 sq ft (56–74 m²)
- Hybrid operating room: 800–1,000+ sq ft (74–93 m²)
Hybrid operating rooms integrate advanced imaging systems such as CT scanners or angiography equipment, which require additional space and structural support.
Proper ceiling height is also important. Most operating rooms require minimum ceiling heights of 3 meters (10 feet) to accommodate surgical lights, imaging equipment, and laminar airflow systems.
3. Functional Zones in an Operating Room
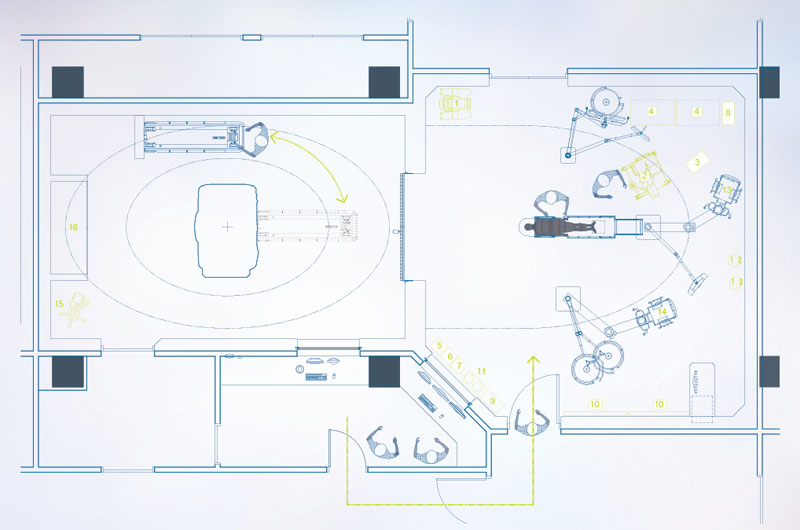
Effective operating room design separates areas based on cleanliness levels and functional use. Most hospitals divide the surgical department into three main zones.
Unrestricted Zone
This is the entry area of the surgical department where street clothes are permitted. It typically includes:
- Reception area
- Patient waiting rooms
- Staff changing rooms
- Administrative offices
Traffic flow begins in this zone before moving toward cleaner areas.
Semi-Restricted Zone
The semi-restricted zone serves as a transition space where staff must wear surgical attire such as scrubs and hair covers. This area includes:
- Equipment storage
- Instrument preparation rooms
- Sterile supply rooms
- Clean corridors
Access is limited to authorized staff.
Restricted Zone
This zone contains the operating rooms themselves and sterile core areas. Strict infection control measures apply here. Staff must wear full surgical attire, including masks.
The restricted zone typically includes:
- Operating rooms
- Scrub areas
- Sterile storage
- Clean supply areas
This zoning system helps control contamination and maintain sterility.
4. Operating Room Layout Types
Different layout configurations are used depending on hospital size, surgical volume, and workflow requirements.
Central Core Layout
In a central core layout, sterile supplies and equipment storage are located in the center of the surgical suite, with operating rooms arranged around the perimeter.
Advantages:
- Efficient access to sterile supplies
- Reduced staff movement
- Improved inventory control
This design is common in large hospitals.
Peripheral Layout
In a peripheral layout, storage areas are located outside the operating rooms along corridors.
Advantages:
- Easier expansion and renovation
- Simpler design for smaller facilities
However, staff may need to travel longer distances to retrieve equipment.
Racetrack Layout
The racetrack layout features two parallel corridors surrounding the operating rooms.
- One corridor for clean supplies
- One corridor for waste and used equipment
This layout improves infection control by separating clean and contaminated traffic.
5. Equipment Placement and Workflow Optimization

Operating rooms contain a large number of devices, including anesthesia machines, surgical tables, monitors, lighting systems, and imaging equipment. Proper equipment placement is essential to maintain an organized workflow.
Key considerations include:
Surgical Table Position
The surgical table is placed at the center of the operating room to allow easy access from all sides. This positioning enables surgeons, nurses, and anesthesiologists to work efficiently.
Anesthesia Workstation
The anesthesia machine is typically located at the head of the patient, providing direct access to airway management equipment and monitoring systems.
Surgical Lighting
Ceiling-mounted surgical lights are positioned directly above the surgical field. Modern lighting systems provide adjustable intensity and shadow-free illumination.
Medical Gas and Power Supply
Operating rooms must be equipped with multiple medical gas outlets, including oxygen, nitrous oxide, and compressed air. Electrical outlets and data connections must also support advanced surgical equipment.
Ceiling-mounted equipment booms are often used to organize cables and equipment, reducing floor clutter and improving safety.
6. Infection Control in Operating Room Design

Infection prevention is one of the most critical aspects of operating room design. The layout and materials used must support strict hygiene standards.
Laminar Airflow Systems
Many modern operating rooms use laminar airflow systems, which deliver filtered air vertically from the ceiling to the floor. This system removes airborne contaminants and reduces infection risks.
HEPA Filtration
High-efficiency particulate air (HEPA) filters are commonly used to remove bacteria, dust, and microorganisms from the air.
Seamless Wall Panels
Seamless wall panels reduce contamination risks because they eliminate joints where bacteria can accumulate. These panels are also easy to clean and disinfect.
Antimicrobial Surfaces
Materials used in operating rooms often include antimicrobial coatings that help prevent microbial growth.
7. Lighting and Visibility
Proper lighting is essential for surgical precision. Operating room lighting systems must provide:
- High brightness levels
- Minimal shadows
- Accurate color rendering
In addition to surgical lights, general ambient lighting helps staff move safely within the room.
Some advanced operating rooms also incorporate integrated display systems that allow surgeons to view medical imaging, patient data, and endoscopic video on large monitors.
8. Ergonomics and Staff Comfort
Surgical procedures can last several hours, making ergonomic design important for medical staff.
Key ergonomic considerations include:
- Adjustable surgical tables
- Flexible equipment positioning
- Adequate space for movement
- Comfortable flooring systems
Proper layout reduces staff fatigue and helps improve surgical performance.
Noise control is another factor. Acoustic ceiling panels and sound-absorbing materials can reduce equipment noise and improve communication among surgical team members.
9. Integration of Advanced Technology
Modern operating rooms are becoming more digitalized and interconnected. Many hospitals now use integrated operating room systems, which allow centralized control of equipment such as:
- Surgical lights
- Cameras
- Video displays
- Medical imaging systems
These systems improve efficiency by allowing surgeons to control equipment through touch panels or voice commands.
Hybrid operating rooms also integrate imaging technologies directly into the surgical environment, enabling real-time diagnostics during procedures.

